Obstructive sleep apnoea in children
What is Paediatric Obstructive Sleep Apnoea (OSA)?
Paediatric obstructive sleep apnoea (OSA) is a condition in which a child’s breathing is frequently blocked during sleep due to partial or complete obstruction of the upper airway. This usually happens because the muscles in the throat relax during sleep, and if the tonsils and adenoids are enlarged, the airway can become obstructed, resulting in pauses in breathing or shallow breathing.
Key Symptoms of OSA in Children:
Snoring: Regular, loud snoring is one of the most common signs.
Mouth Breathing: This can occur day and night, often due to nasal obstruction from enlarged adenoids.
Pauses in Breathing: Sometimes a child may stop breathing for short periods during sleep.
Choking, Gasping, or Snorting: Parents may notice episodes of gasping or snorting while their child is asleep.
Unusual Sleep Positions: Some children sleep in strange positions to help their breathing, like propped up on pillows or with their neck extended.
Restless Sleep: Children may toss and turn more than usual and may sweat excessively.
Daytime Tiredness: Despite adequate sleep time, children may wake up feeling tired or show signs of poor sleep like difficulty concentrating, behavioural problems, or learning issues.
Causes of OSA in Children
Enlarged Tonsils and Adenoids: This is the most common cause. These tissues grow rapidly during childhood and can block the airway during sleep when the muscles relax.
Obesity: Excess weight can put extra pressure on the airway, increasing the risk of OSA.
Nasal Allergies: Conditions like hay fever can worsen airway blockages.
Medical Conditions: Children with conditions like Down syndrome or those with craniofacial abnormalities (e.g. a small jaw) may have a higher risk.
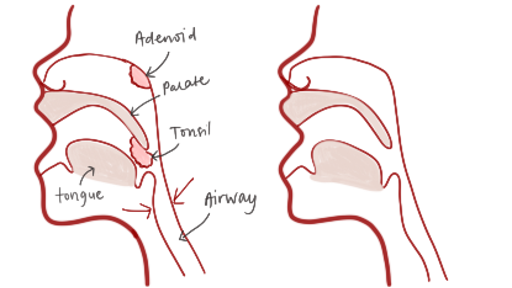
Airway Obstruction in OSA
Normal Airway: The airway remains open during sleep, allowing easy airflow in and out of the lungs.
Obstructed Airway (OSA): Enlarged tonsils or adenoids, along with relaxed throat muscles, can cause the airway to collapse or narrow, leading to breathing difficulties.
Diagnostic Tests for OSA
Overnight Oximetry: A “screening” test that monitors oxygen levels and heart rate during sleep by placing a sensor on the child’s finger or toe. Tests that return with an inconclusive result in a child with persistent symptoms should be considered for a sleep study.
Sleep Study (Polysomnography): This comprehensive test records multiple aspects of sleep, such as breathing, oxygen levels, heart rate, and brain activity. As you can imagine, a child sleeps better in the own homes and in their own beds - we prefer to conduct sleep diagnostics in this environment.
Treatment Options for Paediatric OSA
Nasal Sprays: These can help children with nasal allergies by reducing swelling in the nasal passages or potentially shrink the adenoids.
Adenotonsillectomy: Removal of enlarged tonsils and adenoids is often the first-line treatment and is effective in 80-90% of cases. Most children do not require further treatment after this surgery.
Weight Loss: For overweight or obese children, weight reduction may significantly improve symptoms.
CPAP (Continuous Positive Airway Pressure): In some cases, a CPAP machine is used. It involves wearing a mask over the nose or mouth during sleep, which blows air into the airway to keep it open.
Prognosis In most cases, paediatric OSA resolves after the tonsils and adenoids are removed. However, if symptoms persist or new issues arise, further evaluation and tests may be required.
When to Seek Help
If your child snores regularly, breathes through their mouth, struggles with restless sleep, or shows daytime behavioural or learning difficulties, it may be worth discussing obstructive sleep apnoea with your GP or paediatrician. Early diagnosis and treatment can make a meaningful difference to your child’s sleep, development, and overall wellbeing.
At Prana Paediatric Sleep Service, we provide child-friendly assessment pathways, including home-based sleep testing, to help children sleep more comfortably while still obtaining high-quality diagnostic information.